Patient Care
New York Eye and Ear Infirmary of Mount Sinai (NYEE) is internationally recognized for its outstanding, comprehensive services for the diagnosis and treatment of all diseases of the eyes, ears, nose, and throat and related conditions. Our nurses, physicians, and staff are committed to providing high-quality medical care to every patient who walks through our doors. Because our patients’ convenience and comfort are top priorities, we place an emphasis on less invasive surgical techniques that offer improved success rates and shortened hospital stays. And with a number of children in our care, our specialists coordinate with support staff especially sensitive to the youngest patients and families. This blending of clinical excellence and personalized attention ensures our patients achieve the best possible long-term health.
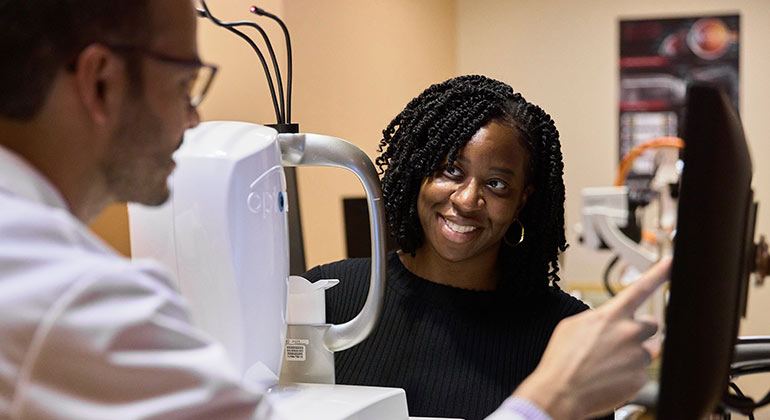
Eye Services
Offering the most advanced care for all eye conditions, including cataracts, glaucoma, age-related macular degeneration, corneal disease, retina conditions, and many other ophthalmologic disorders. Learn More
After-Hours Emergency Eye Care
NYEE’s team of specialists are available for all eye emergencies 24/7, 365 days a year. Learn More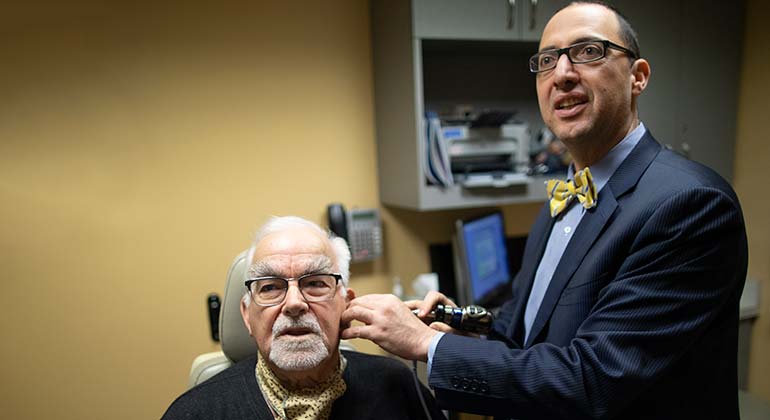
Ear, Nose and Throat Services
Providing leading-edge care for disorders of the ears, nose, throat, sinuses, head, and neck, such as thyroid and parathyroid tumors, sinus problems, voice and throat conditions, hearing disorders, and more. Learn More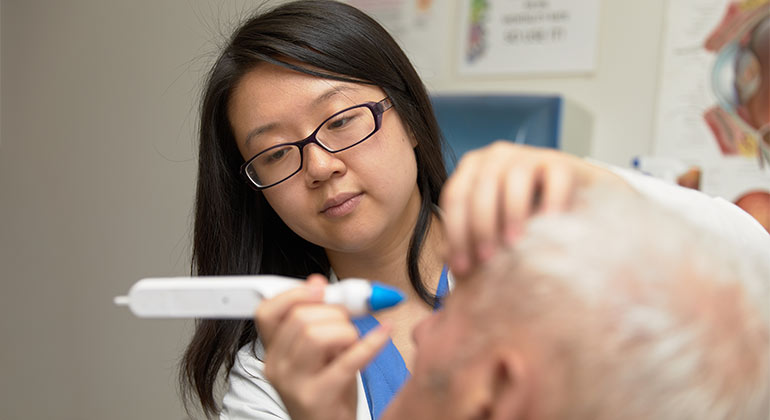
Eye Clinic
The Eye Clinic at New York Eye and Ear Infirmary of Mount Sinai (NYEE) is the place to start when you need to see a doctor for eye injuries and infections. Learn More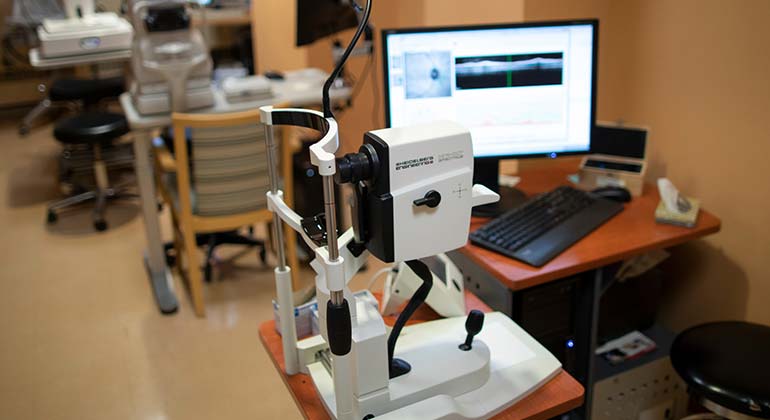
Medical Photography and Imaging Service
Providing a range of advanced radiology, diagnostic imaging, and medical photography services, in order to give physicians the critical information necessary to accurately diagnose your condition and determine the best treatment. Learn More
Optical Shop at NYEE
The New York Eye and Ear Infirmary of Mount Sinai (NYEE) is excited to offer two Optical Shop locations in downtown and uptown Manhattan. Our facilities provide personalized services and offer a wide selection of high-quality eyewear for adults and children. Learn More
Otology Clinic
The dedicated and highly trained physicians and support staff at the ENT Clinic are experts in the treatment of a wide range of ear, nose, and throat disorders, from sinus problems, ear infections, and swallowing disorders to all other general otolaryngology issues. Learn More
Plastic and Reconstructive Surgery
Combining a multidisciplinary approach to cosmetic and reconstructive plastic surgery with the newest technologies in order to ensure the most successful outcomes possible for our patients. Learn More
Sleep Services
Offering comprehensive diagnostic services for patients affected by sleep disorders, including obstructive sleep apnea, snoring, insomnia, narcolepsy, periodic limb movement disorder, and daytime sleepiness. Learn More
